Disclaimer: This writing is intended to serve as a guideline for triaging head and neck injuries that occur during play. If you have any doubts about the safety of the situation, immediately seek professional medical attention.
In rope bondage, injuries happen. No matter how experienced you are as a top or bottom, I can pretty much guarantee you that at some point things will go terribly wrong. The longer you participate in rope bondage, the more likely this is. One of my biggest goals in rope education is helping share information with the community to both prevent and manage injuries. This writing stems from a recent experience I had in rope… and I want to help others who find themselves in a situation like this!
Several months ago, I travelled to visit several play partners of mine in Memphis. We were doing a multi-person suspension shoot on bamboo, and we were on a cement floor. @-EM- had already placed the first bottom in a side suspension. I was going up next, bound in a hip/thigh binder only. My hands were free, likely to be connected later to the third person in the shoot. I lay on the ground, and he dead-lifted me slowly to the maximal height possible with the upline attachment he had chosen. This wasn’t quite lining me up right with the first bottom, so he lowered me, adjusted the up line attachment to the harness, and lifted me again. I used my hands to help press myself upwards and lighten the load. As soon as I was high enough off the ground that I could no longer reach, I lifted my arms and closed my eyes to enjoy the air time. A second or two passed.
All of a sudden, there was a snap and the next thing I realized, I hit the floor head first. Directly on the top of my head. Will all my body weight compressing my head and neck. The upline had snapped.
I moved my hands to the floor beside my head to stabilize myself almost immediately. I rolled/fell from there onto my face. I think -EM- caught my legs. This all happened in a fraction of a second.
I did not lose consciousness.
I was thankfully wearing a posture collar. Why? Because I now have 2 slipped discs in my neck from rock climbing injuries. Thank goodness. It kept my lower neck (where my old injuries are) from hyperextending and further compressing the nerves that are already pinched. But as a result, my upper neck hyperextended instead.
I think -EM- lowered my legs to the ground. I was completely focused on my head and neck. I turned my awareness to my body… I was able to breathe. I could open and close my eyes. I could swallow. I could feel my hands and feet and the cold concrete against my naked body. I wiggled my fingers and my toes. I moved my arms and legs without moving my head or neck. Everything seemed to be working just fine. I said “I’m okay!”
It took a little before I tried moving my head. I did touch my neck first… sore, but not too bad. I rotated my head from side to side very gently and slowly, only about 5-10 degrees in each direction. That was ok. Then I tried shifting my head ever so slightly from side to side, tipping an ear towards each shoulder. That was ok. Then I tried flexing my chin a few degrees towards my chest. Ok. Then I extended my chin slightly away from my chest. Ok. The collar felt very comforting.
Once I had done my head to toe check and my neck check, I carefully sat up and scooted away from the rig so that the others could continue. Of course, they stopped. As soon as -EM- checked in with me and was sure I was stable, he brought the other bottom down. My balance seemed ok.
Then I started assessing my mental status. Was I confused? Could I find the right words and speak clearly? Was I dizzy? Was my memory intact? Were my thoughts clear? Everything seemed amazingly and miraculously ok!
I spoke with the other people present. One got me a blanket, the other got me a bag of ice for my head. The lump was already starting to form. My face hurt. I had a headache.
I took some ibuprofen. I kept my posture collar on… it made me feel safer. It was comforting. -EM- untied me and I put on some clothes.
We spent some serious time assessing the equipment to see what happened. Please see -EM-‘s writing here to see what we found. He and I (and others) have spent quite a bit of time analyzing the failure point, and there is a very important lesson here!
I spent the rest of the evening in close company… constantly watching for any signs of a concussion. All I had was a sore neck and a mild headache and a tender nose and bump on my head. Over the next week, I struggled with a headache on and off and a lot of soreness in my upper neck and my shoulders. I had no issues with my balance. No delayed new neurological symptoms (dizziness, confusion, memory loss, etc…)
I was fine. Just shaken. And thankful that I had been so unbelievably lucky not to have a concussion or a serious neck injury. -EM- and I have been in frequent communication, and we’re both ok. But this was a powerful experience for both of us! We will make some significant changes in our practice of and preparation for rope bondage.
—-
So, what should you take from reading this?
1) This can happen to anyone. He has been rigging for 7 years, and I’ve been bottoming for nearly 4. I’m a doctor. We are both national level presenters in the rope world. We both emphasize safety in all our teaching ventures.
2) If you have a significant injury, take protective measures when doing rope. If I had not been wearing my posture collar, this could have ended in spine surgery.
3) Learn how to triage head and neck injuries!!!
I am going to summarize below some very critical safety information. This does not replace assessment by a trained medical professional. And if you ever have a doubt, dial 911.
Please feel free to share the following guidelines and information with other members of your communities!
—-
1) Head impact is not required to cause a concussion. Shearing forces or sharp jarring movements (ex: transitional suspension, drops, rough body play) can cause just as much damage.
2) If someone is rendered unconscious by the injuring event, DO NOT MOVE THEM! You must assume the have suffered a dangerous neck injury until they regain consciousness. Immobilize the head and neck… you can do this by holding their head firmly between your hands or by placing your hands on their shoulders and securing their head between your forearms. If they are not breathing, or if they do not come back in 30 seconds, you should be dialing 911.
3) Once the person wakes up (or if they did not lose consciousness in the first place), let them know not to move and keep their head and neck immobilized. Start by asking them to move their fingers and toes. See if they have sensation in their limbs. If there are any issues here, call 911! If not, proceed.
4) Next, gently touch the neck to see if there is any significant tenderness. Fracture pain tends to be localized and is often associated with tenderness along the bony bumps on the very back of the neck. Asymmetrical muscle spasms are also condemning. Swelling or deformity of the neck are concerning. If you find any of these red flags, keep the neck immobilized and call 911… there could be a fracture. The person may need full spinal immobilization (like a backboard) to be safely moved. If everything checks out ok, proceed.
5) Ask the person to gently press their head against your hands/forearms without actually moving their head from it’s locked position. This is called “isomeric” testing. If there is severe pain, keep them immobilized and call 911. Otherwise, proceed.
6) Ask them to very slowly and gently move their head… start by rotating a little from side to side. Then try tipping from side to side, like trying to touch one’s ear to the shoulder. Then try flexing (looking down) and extending (looking up). These motions should be no more than 5-10 degrees at first, then it’s ok to increase cautiously if things feel ok. If they feel unstable at all with these motions or their muscles lock up, stop. Immobilize the head and neck. Call 911. If not, proceed.
7) Have them gently move the rest of their body. If their spine and limbs are doing ok and they feel ready to sit up, support them. Check their balance. Can they sit without swaying? Can they stand stable with their arms by their sides? Can they walk in a steady way? Can they walk a straight line? Problems with these things may indicate a concussion.
8) Next, assess mental status. Do they remember what happened? People with concussions are more likely to forget the events immediately preceding the traumatic injury, even though they may know the date and time and where they are. Memory loss often indicates a concussion, but you can have a concussion with any amnesia as well.
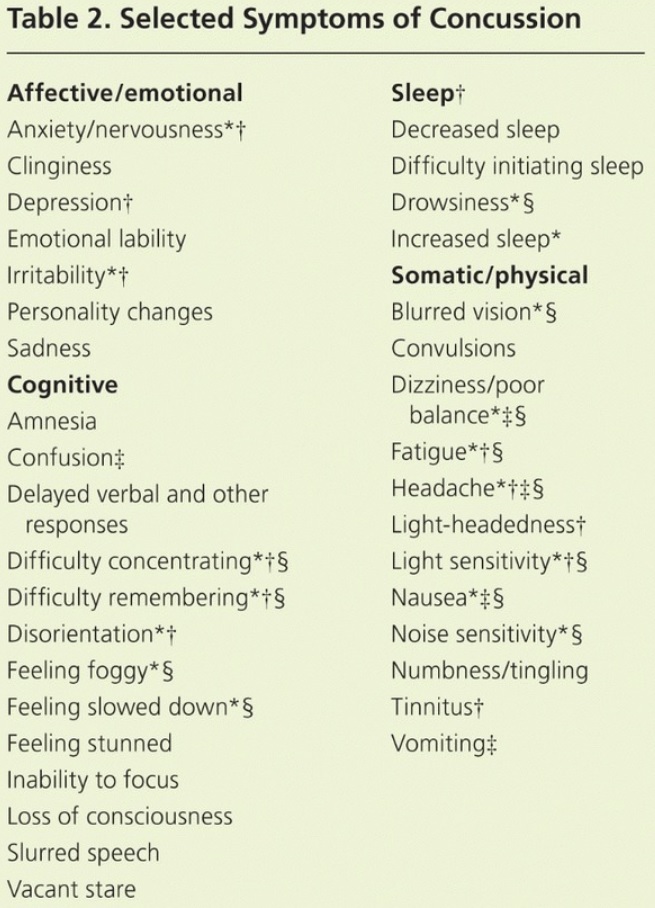
9) Look for other signs and symptoms of concussion. Nausea and vomiting are concerning symptoms of brain swelling and should prompt immediately calling 911. Seizures require immediate evaluation as well. These red flag symptoms may indicate a brain bleed, so do not delay care! At the bottom of this post, I am including a table with symptoms of a concussion. Please watch for all of these things! If multiple of these symptoms are present due more than 15 minutes after the injury, it is important to seek medical care.
10) Continue close surveillance for the next 72 hours. There is a lot of debate about whether someone with a concussion should be awakened frequently to check on them the first night. Ultimately, be sure that you pay close attention for any worsening of the injured person’s condition. New neurological symptoms my indicate a delayed brain bleed or dangerous swelling of the brain. Get help immediately! A headache is to be expected, but a worsening headache is concerning.
11) If you have a concussion, when can you do rope again? The answer will depend on the severity of the concussion, but minimally, you need to wait until ALL the symptoms of the concussion have resolved. If you think you have a concussion, please be sure that a physician is following your progress and clears you before you expose yourself again to the risk of more head injury. Symptoms usually get better in less than 72 hours, and it is rare for them to last more than 10 days. If they do, get help!